what are barriers to evidence based decision making
- Research
- Open Admission
- Published:
A mapping of facilitators and barriers to prove-based direction in health systems: a scoping review study
Systematic Reviews volume 10, Article number:42 (2021) Cite this article
Abstract
Background
Healthcare settings are circuitous, and the decision-making procedure is ordinarily complicated, too. Precise apply of best testify from different sources for increasing the desired outcomes is the consequence of EBM. Therefore, this study aimed to map the potential facilitators and barriers to EBM in health systems to help the healthcare managers to better implement EBM in their organizations.
Methods
The present study was a scoping review (SR) conducted in 2020 based on the integration of the frameworks presented by Arksey and O'Malley (2005) and Levac et al. (2010) considering the Joanna Briggs Found guideline (2015). These frameworks consist of 6 steps. Afterwards finalizing the search strategy, 7 databases were searched, and the PRISMA-ScR was used to manage the retrieval and inclusion of the evidence. Microsoft Excel 2013 was used to extract the data, and the graphic clarification was presented. The summative assay approach was used applying MAXQDA10.
Results
Co-ordinate to the systematic search, 4815 studies were retrieved after eliminating duplicates and unrelated manufactures, 49 manufactures remained to extract EBM facilitators and barriers. Six main aspects mental attitude toward EBM, external factors, contextual factors, resources, policies and procedures, and research capacity and data availability were summarized as EBM facilitators. The barriers to EBM were similarly summarized as mental attitude toward EBM, external factors, contextual factors, policies and procedures, express resources, and enquiry chapters and information availability. The streamgraphs draw that the international attending to the sub-aspects of facilitators and barriers of EBM has been increased since 2011.
Conclusions
The importance of decision-making regarding complex wellness systems, especially in terms of resource constraints and uncertainty weather condition, requires EBM in the wellness system as much equally possible. Identifying the factors that facilitate the use of evidence, likewise every bit its barriers to management and decision-making in the arrangement, can play an important role in making systematic and reliable decisions that can be defended by the officials and ultimately lead to greater savings in organization resources and prevent them from being wasted.
Groundwork
In the last decade of the twentieth century, prove-based medicine was introduced, which is defined equally "the conscientious, explicit, and judicious use of current best testify in making decisions most patient care" [ane]. And then, the concept of evidence use in other areas such as direction was proposed. Data, data, or evidence would be wealth if they have been used for informed decisions [2]. "Evidence-based management (EBM) is about making decisions through the careful, explicit, and judicious use of the all-time available evidence from multiple sources by asking, acquiring, appraising, accumulation, applying, and assessing to increase the likelihood of a favorable event" [3]. Conclusion-making is the core of managerial tasks, so information technology can exist said that evidence-based decision-making (EBDM) is a subset of EBM.
Healthcare settings are complex; consequently, the types of decisions that must exist made are usually complicated too. Often, decisions are based on incomplete and outdated information and personal experiences [iv]. Therefore, using prove in the determination-making procedure can pb to improving the quality of managerial decisions [5]. Managers should make effective and efficient decisions that lead to amend productivity of the organization [1], and the accurate and precise apply of best evidence from unlike sources for increasing the outcomes is the result of EBM [6].
Although some studies have shown that health leaders have a generally positive attitude toward EBM [i], it was applied less than bear witness-based medicine in wellness organizations, so far. Managers do not want in applying show because of existing different barriers [seven], and they cannot overcome these barriers and provide the facilitators to improve implementation of EBM in their organisation until they know and recognize all the possible EBM barriers and facilitators [8, 9].
Recognizing the facilitators and barriers of EBM is necessary to develop this approach and implement it by the health care managers [10]. All the same, several studies were performed to identify facilitators and barriers to EBM or EBDM in healthcare organizations; they simply focused on some aspects of just i or ii of these factors and did not nowadays a comprehensive and complete set up or framework for them [xi,12,13,fourteen,15,sixteen]. Therefore, providing a complete map of the EBM facilitators and barriers in health systems tin provide a comprehensive view that tin help prioritize future efforts and promote the implementation of EBM in the wellness systems [17]. Hence, the main purpose of this written report was to develop a map of the potential facilitators and barriers to EBM in wellness systems. So, we decided to map the EBM facilitators and barriers in wellness systems using scoping review considering of the broad nature of scoping reviews that make them particularly useful for bringing together evidence from disparate or heterogeneous sources and presenting a comprehensive set or framework for desired factors and conditions [18].
Methods
This was a scoping review conducted in 2020. In guild to blueprint the report, the Joanna Briggs Establish'southward protocol (2015) was applied, and the integration based on the frameworks presented by Arksey and O'Malley (2005) [18] and Levac et al. (2010) [19] was used. This slice of the manual, every bit nosotros said, has compared the proposed stages as a framework of scoping review by Arksey and O'Malley [18] and the enhancements suggested by Levac et al. [19]. These frameworks consist of 6 steps. We have tried to compare and integrate these two approaches for a amend analogy of mapping the evidences. Also, the PRISMA-ScR was used as a checklist to report this scoping review (run into supplementary files ane). The detailed methodology of the scoping review is indicated equally follows:
Selecting the research question
In this step co-ordinate to the Joanna Briggs Found manual for scoping reviews (2015), the main enquiry question was defined as "what are the EBM/EBDM facilitators and barriers in health systems/organisation?" As the nature of the scoping review's question is iterative, the specific questions were made as follows:
-
What are the facilitators or enablers that help health systems decide according to the evidence?
-
What are the barriers or limitations to evidence-based decision-making or evidence-based management in health systems?
In this regard, Levac et al. [19] have enhanced the "identifying the research question" to "clarifying and linking the purpose and research question," so after defining the research question, the link between the purpose and the inquiry question was clarified.
Furthermore, the scoping review question guides and directs the development of the specific inclusion criteria for the scoping review. The clarity in the review question assists to develop the protocol, facilitate effectiveness in the literature search, and provide a articulate construction for the development of the scoping review report. Every bit with the title, the question should contain the PCC elements (population, concept, and context) [19]. In this study, the population (P) included all the manufactures considering the facilitators or enablers of the EBM in health systems and those regarding the barriers, obstacles, or limitations of applying EBM in health systems. The concept (C) was the EBM in wellness systems, and the context (C) was all the health organizations, health care centers, and health systems that need evidence to behave and decide.
Searching for related studies
In this footstep, the authors have searched the 7 main databases including Cochrane, ISI spider web of science, PubMed, Scopus, Science Directly, ProQuest, and EMBASE applying related keywords. The search duration was defined from January 01, 2000, up to Baronial 25, 2020. Table 1 shows the finalized search strategy of the scoping review. According to Levac et al. [19] in this step, the feasibility and comprehensiveness of the scoping review were considered, and the seven pre-stated databases were finalized to be searched.
Selecting and refining the studies
The inclusion criteria consisted of those articles in any formats of review, original articles, or dissertations with the English language language that had a full text and was determined or identified facilitators or barriers of EBM in health systems. As well, the exclusion criteria were the studies without total text or English linguistic communication and some types of articles like a volume review, opinion manufactures, or commentaries that had no divers framework for inspecting this report'southward intended factors. In improver, the studies that were conducted clinically regarding the various scopes of health, medicine, or diseases were excluded. During this stride, it was attempted to inquire about the related gray literature or studies that were not included in the search process as far every bit possible by reviewing the reference lists of the selected studies or by contacting some experts or the authors of the articles. This complementary search was based on the related manufactures' titles in the reference lists of the selected articles conducted in Google scholar.
Afterward searching the studies from all databases and eliminating duplicates, the studies were independently reviewed and screened by 2 members of the research team (TSH and MRAM) in three phases by championship, abstract, and and then the total text of the manufactures. At each stage, the terminal determination to include the testify was based on agreement, and in case of disagreement, the opinion of the third member (PB) was used. The Mendeley software (version 1.19.4) was used to manage the procedure of systematic search. At the aforementioned time, the Preferred Reporting Items for Systematic Reviews and Meta-Analyses-extension for Scoping Review (PRISMA-ScR) [20] was applied to manage the process of including the related bear witness (see supplementary files one for PRISMA-ScR checklist and Fig. 1 for PRISMA menses Diagram). Since in the scoping review, appraising the quality of the searched studies is not obligatory [21], the quality of the obtained studies was not appraised via the standard guidelines. However, as it was clarified earlier, the third member (PB) finally screened full-text studies for eligibility, adhering to those same criteria and the relevance of the included studies aims. Every bit it is obvious via this detailed process in the third step, nosotros have both determine the arroyo of selecting the studies and excluding the data according to the third footstep of Levac et al. [19] and Arksey and O'Malley [18] as well.

The PRISMA menses diagram for manufactures' selection
Analyzing and tabulating key data
This step is defined every bit charting the data in the protocol of Arksey and O'Malley and the incorporation of a numerical summary and the qualitative assay via Levac et al. [19] approach. To cover both, in this step, afterwards selecting the concluding studies based on the desired inclusion and exclusion criteria, data on the facilitators and barriers of EBM in health systems were extracted and included in data extraction forms applying Microsoft Excel 2013. The first author'southward proper noun, place, time of the publication, aim of the study, study design, and the report setting were included in the data extraction form. The results of this stride are described in Tabular array 2 in Additional file two. At the same time, for better illustration of the bear witness, the streamgraphs were drawn applying www.plotdb.com.
Then, for qualitative summative assay, the included data was reviewed several times to be assured of considering all large or small sections of the included texts. The aim of the summative analysis is to comprehend all the circuitous subjects and contents of the text associated with the context [22]. Applying this method of analysis in this step helped us to develop and summarize the primary aspects related to the facilitators and barriers of EBM and analyze the primal meaning of a text and its properties.
Summarizing and reporting
At this step, two researchers (TSH and MKRZ) independently integrated and summarized the texts to reach the main and sub-aspects related to the facilitators and barriers of EBM. At the times of probable disagreements, the third person in the research team (Atomic number 82) who has more reflexivity helped to attain the consensus. These aspects then were divers, clarified, and tabulated equally a comprehensive set of all facilitators and barriers to EBM in health systems and organizations (Tables iii and 4 in Additional file 2). The qualitative software MAXQDA version 10 was applied in this step. In this regard via the fifth step, the aim to identify the implications for practice and the policymakers equally well was conducted via the testify summative analysis. This is the indicate that Levac et al. [19] mentioned in their protocol.
Consulting with the experts
This step was mentioned optional according to Arksey and O'Malley. Although the revised protocol by Levac et al. [19] emphasized that achieving the viewpoints of the experts via consultation tin be a required and necessary component. For solving the disharmonize amongst the approaches and achieving an illustrative map of the facilitators and barriers of EBM, we have obtained the consultation of some of the national experts on the finalized tabulated results.
Results
Based on a systematic search, 4815 studies were institute from 7 databases, reaching a total of 2460 articles afterwards duplicates were removed. After excluding studies with unrelated titles, 991 studies remained, and after studying the abstracts and removing unrelated articles, 268 manufactures were selected for the total-text screening. Afterwards studying the full text of the remaining papers, 49 papers were somewhen selected to extract facilitators and barriers to EBM in health systems (Fig. 1).
Most of the studies are (22 (44%)) conducted between 2011 and 2015, 15 (30%) of them conducted between 2016 and 2020, 8 (16%) of them between 2006 and 2010, and the others (4 (eight%)) conducted between 2000 and 2005. Additionally, nearly of the selected articles were from the United states of america (16 (32%)), Canada (11 (22%)), and Australia (6 (12%)). Also, there were 5 (10%) studies from Iran, and the rest (eleven (22%)) were from other countries. Considering the design of the studies, 24 (48%) were qualitative, 18 (36%) were quantitative, and 7 (14%) were mixed-method researches. A summary of the final selected manufactures is given in Table 2 in Additional file 2.
Results of the summative analysis have shown that half dozen chief aspects attitude toward EBM, external factors, contextual factors, resources, policies and procedures, and research capacity and information availability were summarized as EBM facilitators. These six aspects were classified into 24 sub-aspects presented in Table iii in Additional file 2 (meet supplementary files two at the end of the text). Other results of the summative assay have demonstrated that the barriers to EBM were similarly summarized every bit attitude toward EBM, external factors, contextual factors, policies and procedures, limited resources and enquiry chapters, and data availability. These EBM barriers' main aspects in health systems were besides classified into 27 sub-aspects presented in the Table 4 in Boosted file 2 (run into supplementary files ii at the end of the text). Definition and clarification of the concept achieved past the summative analysis have alleged that factors that contributed to the development and implementation of EBM in the arrangement among the included texts were categorized as facilitators and factors that prevented or hindered the promotion of EBM in the organization among the retrieved texts were classified as barriers.
Also, the framework of facilitators and barriers of EBM in health systems is illustrated in Fig. ii. Additionally, the full general tendency of facilitators and barriers of EBM in wellness systems and comparison of the quantity and publication year of the retrieved studies according to the master aspects and sub-aspects of EBM facilitators and barriers are illustrated in Figs. 3, four, and 5, respectively. As it is obvious in these streamgraphs, the international attending to the sub-aspects of facilitators and barriers of EBM has been increased since 2011, and all the sub-aspects were included in different studies from that period.
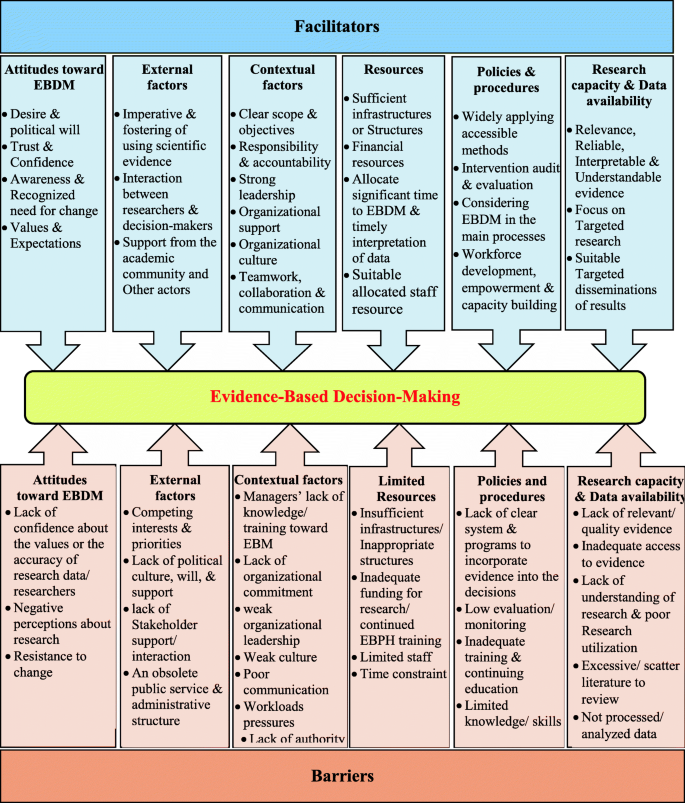
The framework of facilitators and barriers of EBM in health systems
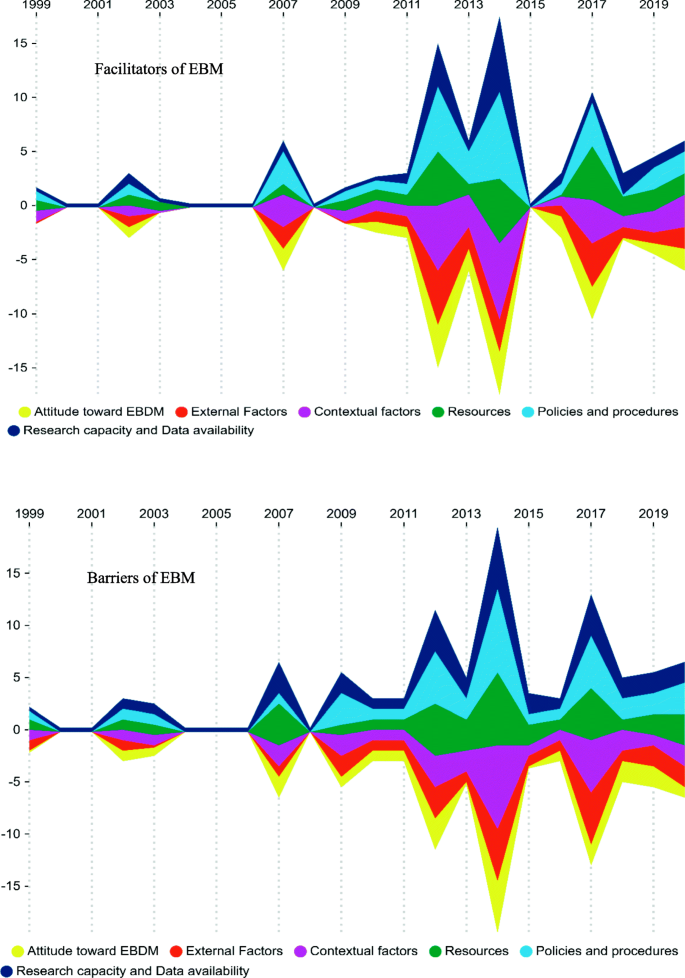
The full general trend of the facilitators and barriers of EBM in health systems

Comparison of the quantity and publication year of the retrieved studies according to the main aspects and sub-aspects of EBM facilitators
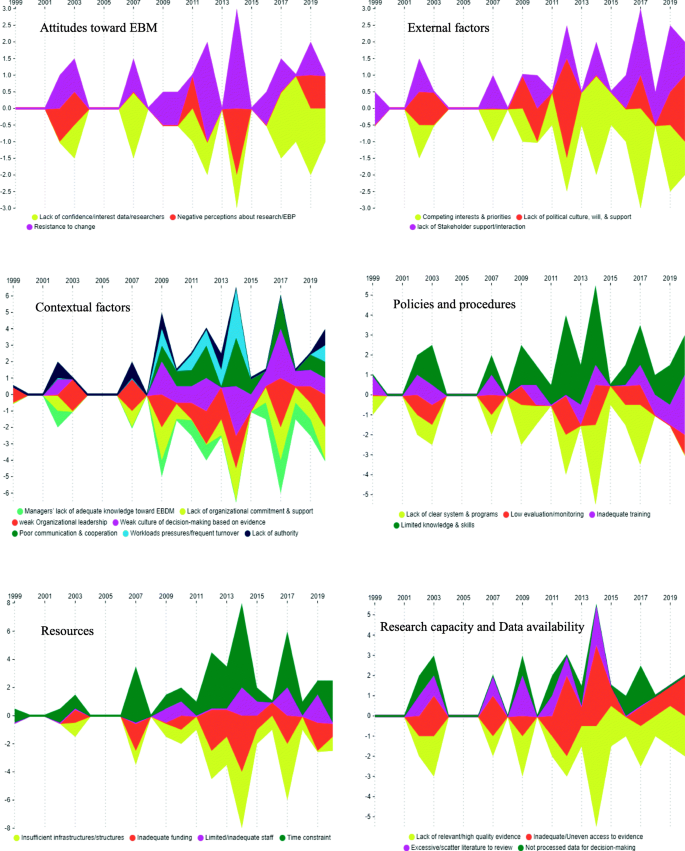
Comparison of the quantity and publication twelvemonth of the retrieved studies according to the main aspects and sub-aspects of EBM barriers
Discussion
In the present written report, we provide a comprehensive map of the facilitators and barriers to EBM in health systems that have been classified into six main aspects including "attitudes toward EBP and research," "external factors," "contextual factors," "policies and procedures," "resources," and "inquiry capacity and information availability". In a study, facilitators and barriers to evidence utilise in programme direction and determination-making within health care organizations were divided into four distinct groups: informational, organizational, individual, and interactional [10]. Another study revealed seven themes to describe both barriers and facilitators: training, attitudes, consumer demand, logistical considerations, institutional back up, policy, and prove [xv].
In this regard, however, several studies were conducted to identify facilitators and barriers of EBM or EBDM in wellness organizations; they but focused on some aspects of just one or two of these factors and did not present a comprehensive and complete set or framework for them [11,12,thirteen,xiv,15,16].
In the following, we discussed the main aspects in two full general categories of facilitators and barriers to EBM.
EBM facilitators
In this inquiry, EBM facilitators were categorized into six primary aspects and 24 sub-aspects. Humphries et al. divided facilitators into five principal themes (information, structure and process of the organization, civilization of the organisation, and individuals' skills and interactions), and 15 sub-theme [ten]. Jessani et al. mentioned nine domains for facilitators (financial, time, work civilization, networks, experience, instructional reputation, geographic location, other actors, and relevance) [23]. Sosnowy et al. divided factors affecting EBDM into two main scopes: internal and external factors with themes such as strong leadership, workforce capacity, resources, funding and programme mandates, political back up, and access to data and programme models suitable to community conditions [24]. In this regard, some of the differences in the categorization of the EBM or EBDM facilitators may be due to the type, scope, extent, and primary objectives of the studies. As well, the unlike attitudes of the authors tin lead to the various classification of the factors. However, none of the previous studies did present a complete and comprehensive classification of the factors that facilitate the development and implementation of EBM in the health system or had non examined the trend or recurrence of these affecting factors on EBM.
Attitudes toward EBM
In the "attitudes toward EBM" aspects, four sub-aspects that were identified the about frequent ones based on the previous studies were "use of bear witness as an organizational value" (14 (28.5%)) and "desire and political will" (13 (26.5%)). Schleiff et al. in their written report explained that EBDM does not take place in a depoliticized vacuum. Political alliances and priorities, knowledge brokers, and other factors take a substantial office to play in applying EBM in health organizations. Hence, after the leaders determined the testify priorities, they tin can identify processes for their generation and use them by using political commitments to ready up structures to support information technology [17].
External factors
In this aspect, the most mentioned sub-aspects were "interaction between researchers and decision-makers and participatory decision-making" (12 (24.five%)). This interaction assists to create consensus betwixt researchers and managers or conclusion-makers, which can facilitate and promote evidence use [ten, 14, 25,26,27,28,29,30,31,32]. The relationship betwixt researchers and decision-makers leads to making decisions on more than accurate, reliable, and up-to-appointment information and thereby avoid waste material of limited resources. Building or strengthening partnerships with schools, hospitals, community and social services organizations, individual businesses, universities, and law enforcement tin can increment EBM in organizations, likewise [30].
Contextual factors
Among six sub-aspects of the "contextual factors" aspect, "potent leadership" (23 (47%)), "organizational/administrative support" (22 (45%)), and "teamwork, collaboration, and advice" (21 (43%)) were the about repeated concepts in the literature. Encouragement of decision-makers to employ evidence in their controlling process can be considered as a alter in organizations. Strong leadership and organizational support are the crucial components of a successful change in any organisation [33]. On the other hand, proactive leadership can be associated with a more positive attitude toward bear witness-based exercise (EBP) [34]. Provision of incentives and motivations [2, 10, 17, 27, 28, thirty, 35, 36] and explicit endeavour to capture synergies betwixt various components of the organizations [28] past a strong and determined leader are the deportment that can encourage the members to focus more on the EBM. As well as, presence of multidisciplinary, diverse management teams [xxx], virtual communication networks [29, 32, 35], interactive web-based coming together (webinars) [35], face up-to-face up meetings [28, 30] and brainstorming [10, 29], and use of common language and terminology [thirty] tin can facilitate teamwork and consequently heighten the utilise of evidence in the controlling procedure in the organizations.
Resources
This aspect included 4 sub-aspects, and among them, "sufficient infrastructures or structures" was the almost mentioned sub-aspect (24 (49%)) in the studies. In this regard, some factors such every bit information systems [2, 27, 28, 30, 35] and technical infrastructure [2, 14, 28, 37]; appropriate wireless, internet, and intranet admission and computers [xiv, xvi, 17, 28, 29]; digitization of datasets, reports, and processes [17]; access to research and library services [10, 12, 36, 38,39,40,41,42, thirteen, 14, 17, 25, 27, thirty, 32, 35]; noesis on management tools [25, 30, 38, 39]; and the existence of a section for quality assurance [28] tin can have a great bear on on providing the necessary infrastructure for EBM and promoting it in the organization.
Policies and procedures
This aspect included four sub-aspects. "Workforce development, empowerment and training leaders/staff" was the nearly frequent sub-aspect (31 (63%)) in this aspect. Empowering the conclusion-maker and building chapters to apply bear witness in the controlling process can lead to more usage of evidence in an arrangement. Besides, evaluating the implementation of the decisions taken tin can lead to reinforcing and institutionalizing the use of EBM in the organization. Considering this, some factors such as "executive grooming programs" [2, 27, 30, 39], "leadership training" [25, 30], "offer the organisation every bit a learning laboratory for Ph.D. and other senior students" [43], "increasing number of graduate programs that incorporate training in empirically supported treatments" [15], "comport interactive workshops" [28, 44], "consultations" [44], "sending staff to external training programs," "adapting training to specific specialties or clienteles" [28], "in-service and multidisciplinary preparation," and "skills-based training" [30] tin can better EBM. Decision-maker needs to learn how to gather and assess bear witness [v]. Training the individuals virtually EBM may enrich their attitude and understanding of the importance of EBM [fourteen].
Enquiry capacity and information availability
In this aspect, three sub-aspects have existed. Accordingly, "relevance, reliable, interpretable and understandable prove" was the most mentioned sub-aspect (10 (20%)) in studies. Evidence is the fundamental role of EBM, so the data for use should exist real-time, synthesized, and from different agencies [17], and if and then, the managers tin brand good decisions. Without this information, wrong decisions volition be made, and it can lead to non only the system that does non improve but may push information technology away from its desired goals.
EBM barriers
Different types of factors were explained which tin can impede the development of EBM in the organization. In this research, the identified barriers in literature are divided into six main aspects with 27 sub-aspects. Liang et al. identified 12 barriers in three levels including a broader level, organization, and private manager [27]. Humphries et al. identified five main themes (information, the construction and process of the organization, the civilization of the organization, and individuals' skill and interaction) and 28 sub-themes [10]. Pagoto et al. identified six themes for barriers: attitude toward EBP, training, logistical, policy, evidence, institutional support, and consumer demand [15] which is somehow similar to this study. Majdzadeh et al. mentioned three chief themes (decision-makers' characteristics, decision-making surroundings, and research system) and 14 sub-themes for EBDM barriers in Islamic republic of iran's wellness system [45]. Again, none of the previous studies most the barriers of the EBM in health systems did present a complete gear up of factors. Moreover, it seems that the type, scope, extent, and main objectives of the studies and also the different attitude of the authors leads to the various classification of the factors.
Attitudes toward EBM
In this aspect, both the "resistance to change" (xiv (28.5%)) and "lack of confidence/interest about the values or the accurateness of inquiry data or the researchers" (xiii (26.5%)) were most repeated in previous researches. Adaption to various changes in organizations is unavoidable [46]. Resistance to alter may be due to inappropriate apply of power, challenges to cultural norms and institutionalized practices, lack of understanding, inappropriate timing, inadequate resources, incorrect information, or employees' suspicion of honorable management intentions [47]. Moving toward EBM is considered every bit a change in an system that causes fear for the managers or staff. Fearfulness of change toward the unknown leads to resistance to change, so proper strategies and policies such as training, education, or compensations are essential to successful changes [46].
External factors
In the "external factors" aspect, "competing interests and priorities" which is defined as "the need for a bureaucracy of approaches that allow to competing for organizational priorities and a balance betwixt reactive and proactive management" [48] was most cited (17 (35%)) in the literature. It was explained in the studies that oftentimes centralized [49], heterogeneous [31], or politically influenced decisions [10, 50] might forestall the managers of the wellness organizations from making efficient decisions based on the all-time available bear witness.
Contextual factors
Among the "contextual factors," "weak Organizational leadership" (20 (41%)) and "weak culture of conclusion-making based on evidence" (18 (37%)) were the near repeated sub-aspects in the literature. It is clear that no program or change in the organisation will be successful without the delivery and support of the leader and senior officials of the system. Also, the implementation of any programme and reforms requires the existence of a suitable cultural context and infrastructure. Civilisation is an important bones chemical element to back up changes in an organization, as well as to move toward EBM [51]. Organizational culture plays a significant role in innovation and changes [52]. Developing a dominant culture for EBM is essential in organizations to ensure that decisions are well appraised past research evidence.
Policies and procedures
In this aspect, "limited knowledge and skills to access, interpret, appraise, and synthesize enquiry evidence, or in research methods or foreign linguistic communication" was the most cited sub-aspect (26 (53%)) by the previous studies. According to a previous written report, inadequate technical training to enable managers to interpret research findings was a barrier to adequate accessibility to scientific evidence [53]. Applying EBM needs to learn how to search and evaluate different evidence critically from scientific findings to experts' opinions and even some economic information, which requires some new managerial skills [5]. Besides, preparation the staff about EBDM can atomic number 82 to not only an understanding of the importance of its implication in the organisation merely also they can larn how to acquire, assess, adapt, and apply researches in the organizational controlling process [14]. Also, Walker et al. stated that librarians could exist a crucial role of improving understanding and use of evidence in the organization by raising sensation of evidence-based resources among the employees. Thus, creating a strong communication between librarians and decision-makers can increase the use of bear witness [54].
Limited resources
"Time constraint for collecting and interpretation of information, engaging in research or implementation of an prove-based conclusion making" was identified as an of import and frequent (33 (67%)) sub-aspect in the "limited resources" aspect. Health workers are overworked, and then fourth dimension constraints are one of the barriers to using evidence. Organizations should provide the essential tools to facilitate quick and piece of cake access to the required research, ensuring appropriate journal subscriptions, and providing relevant links on the organizations' intranet [fourteen] to overcome these time constraints to some extent.
Inquiry capacity and data availability
"Lack of relevant or high-quality prove" (24 (49%)) and "inadequate/uneven admission to evidence" (22 (45%)) were the sub-aspects that were mentioned in much other literature. Uncertain/unreliable evidence [40, 42], non-useful format [31], not available data in an extractable format [55], and gaps in evidence [24, 36, 41, 48]/inadequate research findings [xvi] were mentioned by other studies as the items that can preclude the testify-based decisions. Limited admission to the electronic databases and experts' opinions leads to barriers in using evidence in the conclusion-making procedure [42]. Testify is the principal part of the EBDM process; therefore, inadequate admission to evidence tin can make it difficult to go toward EBM.
Conclusion
The importance of controlling regarding complex health systems, especially in terms of resource constraints and dubiety conditions, makes it necessary to apply the EBM in the health system organizations as much as possible. Existence and admission to apparent evidence from a variety of sources can reduce incertitude and stance-based decision-making. Therefore, we tried to provide a comprehensive map of EBM facilitators and barriers in health system organizations since we did not find a study that provided a comprehensive synthesis of all facilitating and hindering factors to EBM. We expect that the authorities and managers of health organisation organizations tin can make evidence-based decisions in their organizations using the map and the consummate set of potential EBM facilitators and barriers presented in this study and past focusing on improving the facilitators and reducing or eliminating the barriers. Such systematic, reliable, and rational decisions can properly justify the stockholders' demands and at the same fourth dimension lead to better use of express resources in the organizations.
Strengths and limitations of the study
The near of import strength of this study is providing a comprehensive ready of EBM facilitators and barriers in health systems and map their trends over years. At the same fourth dimension, the main novelty and contribution to the cognition of the study is the integration of ii methodologies for conducting the scoping review.
Nevertheless, similar whatsoever other review, in this scoping review, some relevant sources of data might have been omitted, and the review was dependent on information on the review question and the selected search strategy. Also, for further studies, it might be interesting to survey the factors provided in this report from the healthcare managers' perspective in different contexts.
Availability of data and materials
Data charting is available as an additional file.
Abbreviations
- EBM:
-
Evidence-based management
- EBDM:
-
Evidence-based decision-making
- EBP:
-
Evidence-based practice
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PRISMA-ScR:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses- extension for Scoping Reviews
References
-
Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS. Evidence based medicine: what information technology is and what it isn't. BMJ. 1996;312(7023):71–2.
-
Belay T, Mbuya Northward, Rajan V. Data utilization and show-based decision making in the health sector: survey of three Indian states. 2009 [cited 2018 May 26]. Available from: https://openknowledge.worldbank.org/handle/10986/3161
-
A definition of testify-based management – center for evidence based management [Cyberspace]. [cited 2020 Sep iv]. Available from: https://cebma.org/a-definition-of-evidence-based-management/
-
Pfeffer J, Sutton R. Difficult facts, dangerous half-truths, and full nonsense: profiting from evidence-based direction. Boston: Harvard Business Press; 2006.
-
Axelsson R. Towards an evidence-based health intendance management. Int J Health Plann Manage. 1998;1751(Baronial):307–17.
-
Janati A, Hasanpoor E, Hajebrahimi S, Sadeghi-Bazargani H. Health care managers' perspectives on the sources of prove in evidence-based hospital management: a qualitative study in Iran. Ethiop J Wellness Sci. 2017;27(6):659.
-
Gautam M. Addressing the enquiry-exercise gap in healthcare management. J Public Heal Manag Pract. 2008;14(2):155–9.
-
Bastani P, Alipoori S, Imani-Nasab MH, Jamalabadi Southward, Kavosi Z. Bear witness-based decision making among healthcare managers: evidence from a developing country. Int J Healthc Manag. 2019;0(0):1–vi. Available from. https://doi.org/10.1080/20479700.2019.1632002.
-
Barends Eastward, Villanueva J, Rousseau DM, Briner RB, Jepsen DM, Houghton E, et al. Managerial attitudes and perceived barriers regarding evidence-based practise: an international survey. PLoS Ane. 2017;12(x):vii–9.
-
Humphries South, Stafinski T, Mumtaz Z, Menon D. Barriers and facilitators to evidence-utilise in program management: a systematic review of the literature. BMC Health Serv Res. 2014;14(1):171 [cited 2018 May sixteen]. Available from: http://bmchealthservres.biomedcentral.com/articles/10.1186/1472-6963-14-171.
-
Greaves DE. Show-based management of Caribbean health systems: barriers and opportunities. Int J Heal Gov. 2017;22(two):104–17 [cited 2018 May 28]. Bachelor from: http://world wide web.emeraldinsight.com/doi/10.1108/IJHG-01-2017-0001.
-
Niedzwiedzka BM. Barriers to evidence-based decision making among Polish healthcare managers. Heal Serv Manag Res. 2003;xvi(2):106–15 [cited 2018 May xix]. Available from: http://journals.sagepub.com/doi/x.1258/095148403321591429.
-
Dodson EA, Baker EA, Brownson RC. Utilize of evidence-based interventions in state health departments: a qualitative assessment of barriers and solutions. J PUBLIC Heal Manag Pract. 2010;16(6):E9–E15.
-
Ellen ME, Léon G, Bouchard K, Ouimet M, Grimshaw JM, Lavis JN. Barriers, facilitators and views about adjacent steps to implementing supports for evidence-informed decision-making in health systems: a qualitative study. Implement Sci. 2014;ix(1):179 [cited 2018 May 28]. Available from: http://implementationscience.biomedcentral.com/articles/10.1186/s13012-014-0179-8.
-
Pagoto SL, Spring B, Coups EJ, Mulvaney South. Barriers and facilitators of testify-based practice perceived by behavioral science health professionals. J Clin Psychol. 2007;63(7):695–705.
-
Ayoubian A, Nasiripour AA, Tabibi SJ, Bahadori K. Evaluation of facilitators and barriers to implementing evidence-based practise in the health services: a systematic review. Galen Med J. 2020;9:e1645. Bachelor from: http://www.embase.com/search/results?subaction=viewrecord&id=L631663192&from=export.
-
Schleiff MJ, Kuan AL, Ghaffar A. Comparative analysis of country-level enablers, barriers and recommendations to strengthen institutional capacity for evidence uptake in controlling. Heal Res Policy Syst. 2020;18(one):12 Available from: https://health-policy-systems.biomedcentral.com/rails/pdf/10.1186/s12961-020-00546-4.
-
Arksey H, O'Malley 50. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(one):19–32.
-
Levac D, Colquhoun H, O'Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010;5(1):one–nine.
-
PRISMA [Internet]. [cited 2020 Sep fifteen]. Available from: http://world wide web.prisma-statement.org/Extensions/ScopingReviews
-
Grant MJ, Booth A. A typology of reviews: an analysis of 14 review types and associated methodologies. Wellness Info Libr J. 2009;26(two):91–108 Available from: http://world wide web.ncbi.nlm.nih.gov/pubmed/19490148.
-
Rapport F. Summative analysis: a qualitative method for social scientific discipline and health enquiry. Int J Qual Method. 2010;ix:270–90.
-
Jessani Northward, Kennedy C, Bennett Southward. A SB-Eastward& P, 2017 U, Bennett S. Enhancing testify-informed decision making: strategies for date between public health kinesthesia and policymakers in Republic of kenya. Evid Policy. 2017;thirteen(2):225–53 [cited 2018 May 28]. Available from: http://www.ingentaconnect.com/content/tpp/ep/2017/00000013/00000002/art00004.
-
Sosnowy CD, Weiss LJ, Maylahn CM, Pirani SJ, Katagiri NJ. Factors affecting evidence-based determination making in local wellness departments. Am J Prev Med. 2013;45:763–eight [cited 2018 May 26]. Available from: http://ovidsp.ovid.com/ovidweb.cgi? T=JS&CSC=Y&NEWS=N&PAGE=fulltext&D=medl&AN=24237920 http://sfx.scholarsportal.info/mcmaster?sid=OVID:medline&id=pmid:24237920&id=doi:10.1016%2Fj.amepre.2013.08.004&issn=0749-3797&isbn=&volume=45&issue=half-dozen&spage=763&pages=76.
-
Spiri WC, Kurcgant P, Pereira MV. Perception of nursing centre managers almost the bear witness-based management. Int Arch Med. 2017;10(February):11 Available from: http://imedicalsociety.org/ojs/index.php/iam/article/view/2311.
-
Moussata CO. Show-based management and its influence on the practices of senior leaders of hospitals in the Denver Metropolitan Area. ProQuest Dissertations and Theses. Ann Arbor: Colorado Technical Academy; 2017. [cited 2018 May 19]. Bachelor from: https://search.proquest.com/docview/1967189422?accountid = 41313
-
MsPZ LM, MsPF HM, MhsMBAPSG LB, MADPG MB. A framework to improve evidence-informed controlling in health service management. Aust Heal Rev. 2012;36(three):284–9 Bachelor from: https://search.proquest.com/docview/1615162414?accountid = 41313.
-
Ellen ME, Léon One thousand, Bouchard One thousand, Lavis JN, Ouimet M, Grimshaw JM. What supports do wellness organisation organizations have in place to facilitate evidence-informed determination-making? A qualitative study Implement Sci. 2013;8(i):84–103.
-
Dobbins M, Jack S, Thomas H, Kothari A. Public health decision-makers' advisory needs and preferences for receiving enquiry evidence. Worldviews Evid Based Nurs. 2007;4(three):156–63.
-
Brownson RC, Allen P, Duggan Thou, Stamatakis KA, Erwin PC. Fostering more-constructive public health by identifying administrative evidence-based practices: a review of the literature. Am J Prev Med. 2012;43(3):309–xix Available from: https://www.scopus.com/inward/record.uri?eid=ii-s2.0-84865688888&doi=10.1016%2Fj.amepre.2012.06.006&partnerID=forty&md5=a843f04e58b619ab9355a98bbfeef51a.
-
Kazman Kohn M, Berta W, Langley A, Davis D. Evidence-based determination making in health care settings: from theory to exercise. In: Advances in health care management: Emerald Grouping Publishing Ltd; 2011. [cited 2018 May 26]. p. 215–34. Available from: http://www.emeraldinsight.com/doi/x.1108/S1474-8231%282011%290000011012.
-
Ward M, Mowat D. Creating an organizational civilization for evidence-informed decision making. Healthc Manag Forum. 2012;25(3):146–l Available from: https://www.scopus.com/inward/tape.uri?eid=2-s2.0-84867778644&doi=ten.1016%2Fj.hcmf.2012.07.005&partnerID=40&md5=42f06b7236a4a1cd6a4739c7e1900764.
-
Ajmal Due south, Farooq Chiliad, Sajid North, Awan S. Role of leadership in change management process. Abasyn Univ J Soc Sci. 2012;5(two):111–24.
-
Powell BJ, Mandell DS, Hadley TR, Rubin RM, Evans Ac, Hurford MO, et al. Are general and strategic measures of organizational context and leadership associated with noesis and attitudes toward evidence-based practices in public behavioral health settings? A cross-exclusive observational report. Implement Sci. 2017;12(i):64.
-
Jacob RR, Baker EA, Allen P, Dodson EA, Duggan K, Fields R, et al. Training needs and suport for EBP descision making in PH workforce-2014.pdf. BMC Health Serv Res. 2014;14(564):1–12.
-
Hasanpoor E, Belete YS, Janati A, Hajebrahimi Southward, Haghgoshayie East. Nursing managers' perspectives on the facilitators and barriers to implementation of evidence-based direction. Worldviews Evid Based Nurs. 2019;16(4):255–62 Bachelor from: http://world wide web.zgddek.com/EN/abstract/abstract24970.shtml.
-
Harris C, Garrubba M, Melder A, Voutier C, Waller C, Rex R, et al. Sustainability in Health care by Allocating Resources Effectively (SHARE) 8: developing, implementing and evaluating an evidence dissemination service in a local healthcare setting. BMC Health Serv Res. 2018;18(one):151–76. Available from: https://www.scopus.com/inward/record.uri?eid=2-s2.0-85042873576&doi=ten.1186%2Fs12913-018-2932-1&partnerID=40&md5=2daa5bbd3ccddf299f7b9d527b6105af.
-
Yost J, Dobbins One thousand, Traynor R, DeCorby 1000, Workentine Due south, Greco L. Tools to support evidence-informed public health decision making. BMC Public Wellness. 2014;14(one):728 [cited 2018 May 28]. Bachelor from: https://bmcpublichealth.biomedcentral.com/articles/10.1186/1471-2458-14-728.
-
Peirson L, Ciliska D, Dobbins Thou, Mowat D. Building capacity for show informed conclusion making in public health: a instance study of organizational change. BMC Public Health. 2012;12(1):137 [cited 2018 May 28]. Bachelor from: https://world wide web.scopus.com/inward/record.uri?eid=2-s2.0-84857132983&doi=10.1186%2F1471-2458-12-137&partnerID=40&md5=68e18844316881fb3f2662477825d441.
-
Wallington SE. Bear witness-based controlling: an integral office of the system of knowledge [Net]. ProQuest Dissertations and Theses. Ann Arbor: Royal Roads Academy (Canada); 2002. Available from: https://search.proquest.com/docview/305484310?accountid=41313
-
Harris C, Allen K, Waller C, Dyer T, Brooke V, Garrubba M, et al. Sustainability in Health intendance by Allocating Resources Effectively (SHARE) 7: supporting staff in bear witness-based conclusion-making, implementation and evaluation in a local healthcare setting. BMC Wellness Serv Res. 2017;17(1):430 [cited 2018 May 19]. Available from: http://bmchealthservres.biomedcentral.com/articles/ten.1186/s12913-017-2388-eight.
-
Armstrong R, Waters E, Moore L, Dobbins Thousand, Pettman T, Burns C, et al. Understanding bear witness: a statewide survey to explore bear witness-informed public health decision-making in a local authorities setting. Implement Sci. 2014;9(1):188 [cited 2018 May 28]. Available from: http://implementationscience.biomedcentral.com/articles/10.1186/s13012-014-0188-7.
-
Ward Thousand, Mowat D. Creating an organizational culture for evidence-informed decision making. Healthc Manag Forum. 2012;25(3):146–50.
-
Vratny A, Shriver D. A conceptual model for growing evidence-based. Nurs Adm Q. 2007;31(two):162–seventy.
-
Majdzadeh R, Yazdizadeh B, Nedjat S, Gholami J, Ahghari South, R. Thou, et al. Strengthening evidence-based decision-making: is it possible without improving health arrangement stewardship? Health Policy Plan. 2012;27(6):499–504 [cited 2018 May 15]. Bachelor from: https://academic.oup.com/heapol/commodity-lookup/doi/10.1093/heapol/czr072.
-
Agboola AA, Salawu RO. Managing deviant behavior and resistance to change. Int J Business Manag. 2011;6:235–42.
-
Graetz F, Rimmer Grand, Lawrence A, Smith A. Managing organisational alter. Commonwealth of australia: John Wiley & Sons; 2006.
-
Addison PFE, Cook CN, de Bie 1000. Conservation practitioners' perspectives on conclusion triggers for show-based management. Bennett J, editor. J Appl Ecol. 2016;53(five):1351–7 [cited 2018 May 28]. Available from: http://doi.wiley.com/10.1111/1365-2664.12734.
-
Bowen S, Erickson T, Martens P, Crockett Due south. More than " Using Enquiry ": the real challenges in promoting testify-informed decision-making plus. Heal Policy. 2009;four(3):87–102 Available from: http://www.ncbi.nlm.nih.gov/pmc/manufactures/PMC2653695/.
-
Oronje RN, Murunga Six, Zulu EM. Strengthening chapters to use enquiry bear witness in health sector policy-making: feel from Kenya and Malawi. Heal Res Policy Syst. 2019;17(1):101. Available from: http://www.embase.com/search/results?subaction=viewrecord&id=L630287856&from=consign.
-
Damschroder LJ, Aron DC, Keith RE, Kirsh SR, Alexander JA, Lowery JC. Fostering implementation of health services research findings into do: a consolidated framework for advancing implementation science. Implement Sci. 2009;4(1):50.
-
Abdi K, Senin AA. Investigation on the impact of organizational civilisation on organisation innovation. J Manag Policies. 2014;2(ii):1–10.
-
Giehl ELH, Moretti Yard, Walsh JC, Batalha MA, Cook CN. Scientific evidence and potential barriers in the management of Brazilian protected areas. PLoS I. 2017;12(i):e0169917.
-
Barr-Walker J. Evidence-based data needs of public wellness workers: a systematized review. J Medi Library Assoc. 2017;105:69–79.
-
McDiarmid M, … SK-J of the, 2007 U, of the … SK-J, undefined 2007, … SK-J of the, et al. Bear witness-based authoritative determination making and the Ontario infirmary CEO: information needs, seeking behaviour, and access to sources. ejournals.library.ualberta.ca [Internet]. [cited 2018 May 28]; Available from: https://ejournals.library.ualberta.ca/index.php/jchla/article/viewFile/24060/17884
Acknowledgements
This research, derived from Proposal No. 96-01-07-14184, was conducted past Mrs. Tahereh Shafaghat as part of the activities required for a Ph.D. degree in health care direction at the Shiraz University of Medical Sciences. The authors wish to express their sincere gratitude to the inquiry assistants of Shiraz University of Medical Sciences for its fiscal and administrative support.
Funding
As the overall study was an canonical research project of Shiraz University of Medical Sciences and was conducted by Mrs. Tahereh Shafaghat as role of the activities required for a Ph.D. caste in the wellness care management field, this study was supported past the Shiraz Academy of Medical Sciences. This study was sponsored by Shiraz Academy of Medical Sciences under code (97-01-07-18586). The funding body was not involved in the design of the study, information collection, assay, and estimation, likewise equally in writing the manuscript.
Author information
Affiliations
Contributions
TSH under the supervision of PB designed the study and its overall methodology. Pb edited and finalized the commodity. TSH searched all the databases and with the help of MRAM retrieved the sources and scanned and screened all the manufactures in 3 phases. TSH also prepared the draft of the article. MAB and MKRZ contributed to data analysis. Likewise, the report was nether consultation and supervision past ZK and MHIN as advisors. All the authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This written report is approved by the Shiraz University of Medical Sciences ideals committee with the ID number of IR.SUMS.REC. 18586.
Consent for publication
Not applicable.
Competing interests
The authors declare that they take no competing interests.
Additional information
Publisher'due south Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1.
Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklist.
Additional file two: Table 2.
Summary of characteristics of included studies. Table 3. The facilitators of EBM in health systems. Table 4. The barriers of EBM in health systems management.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in whatever medium or format, equally long as yous give appropriate credit to the original writer(s) and the source, provide a link to the Creative Commons licence, and signal if changes were made. The images or other tertiary party material in this article are included in the article's Artistic Commons licence, unless indicated otherwise in a credit line to the material. If fabric is not included in the commodity's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you lot will demand to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Artistic Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the information made bachelor in this commodity, unless otherwise stated in a credit line to the data.
Reprints and Permissions
Near this article
Cite this commodity
Shafaghat, T., Imani Nasab, Grand.H., Bahrami, M. et al. A mapping of facilitators and barriers to testify-based management in health systems: a scoping review study. Syst Rev 10, 42 (2021). https://doi.org/ten.1186/s13643-021-01595-8
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/10.1186/s13643-021-01595-8
Keywords
- Evidence-based decision-making
- Facilitators
- Barriers
- Health organization
Source: https://systematicreviewsjournal.biomedcentral.com/articles/10.1186/s13643-021-01595-8
0 Response to "what are barriers to evidence based decision making"
Post a Comment